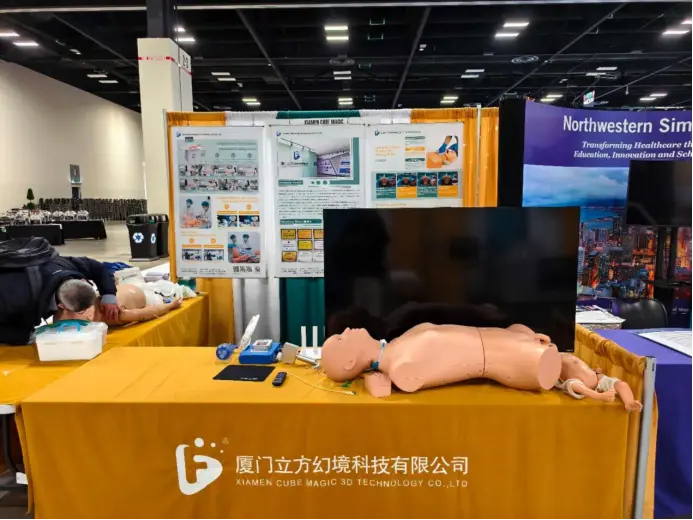
New Trends in Medical Education 2025: Smarter Human-Simulator Integration for Efficient Training
1. AI-Powered Scenario Generation & Feedback
One of the big breakthroughs is using large language models (LLMs) and AI systems to auto-generate simulation scenarios and provide formative feedback. Instead of educators handcrafting each case, AI can tailor scenarios to learner performance, fill gaps, and even simulate branching dialogues.
-
For example, a recent study “Automated Generation of High-Quality Medical Simulation Scenarios” proposes integrating semi-structured clinical data with LLMs to create scenario variants automatically.
-
Another platform, MedSimAI, uses AI to simulate patient encounters and immediately give structured feedback to learners (e.g. interview skills).
This approach reduces faculty overhead, ensures consistency, and lets learners drill many more cases without human limitation.
2. Hybrid / Digital — Beyond Physical Manikins
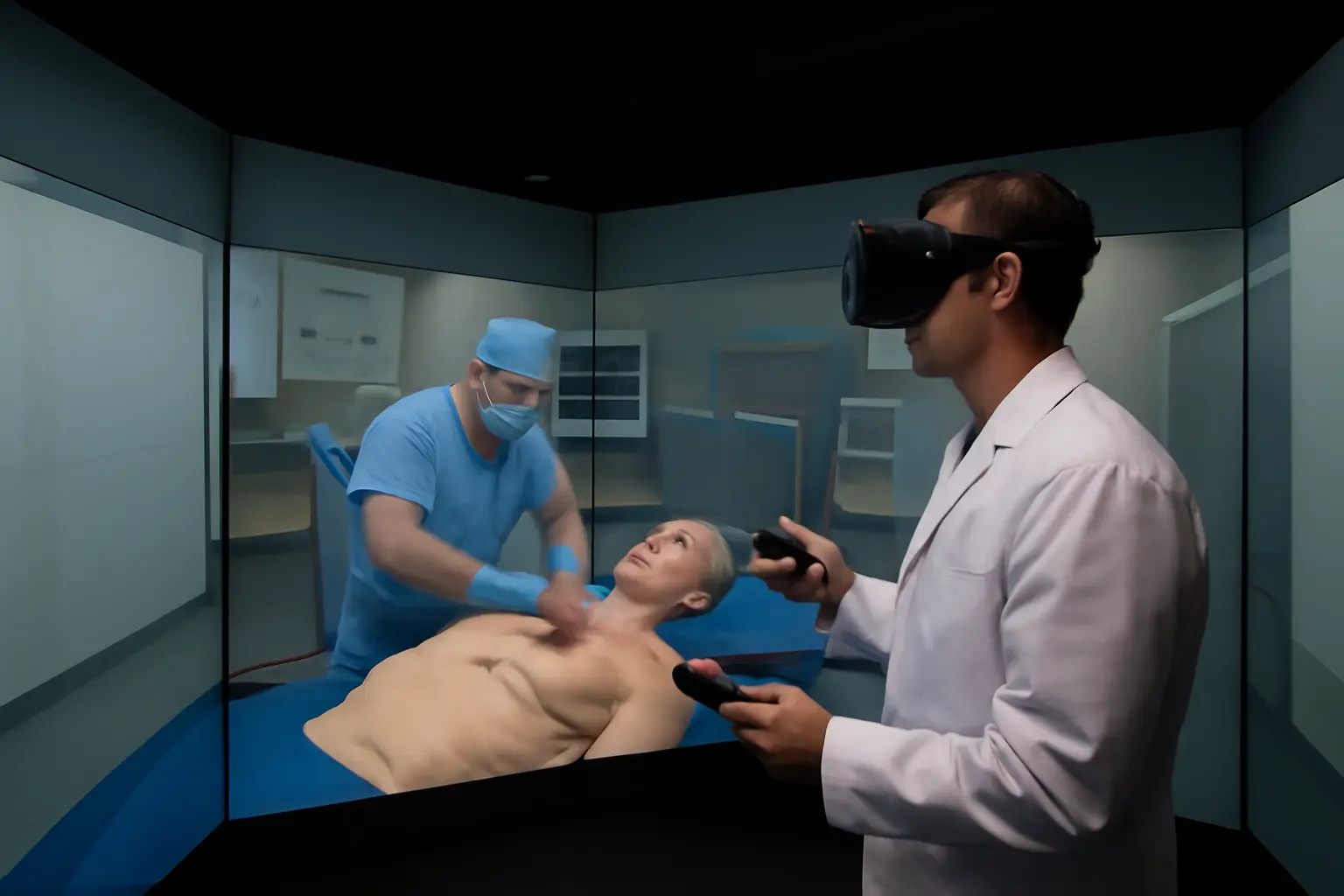
While high-fidelity mannequins remain important, the trend is shifting toward combining physical simulators with virtual / augmented reality (VR/AR) or digital twins:
-
Simulation research shows that the field is gradually moving from purely physical models toward virtual, digitally-based simulations and online education.
-
Mixed Reality and digital-physical twins are emerging. For instance, a recent study built apatient-specific dynamic digital-physical twin for coronary intervention training, combining real anatomy models with virtual simulation.
-
The global market report also points to increasing use of augmented reality, advanced procedural simulators, and 3D printing in simulation design.
The advantage? Students can train on virtual models (e.g. accessible remotely) and then transition to physical simulators with more realism.
3. Competency Tracking, Big Data & Analytics
Moving beyond “one-off skills practice,” educators are embedding competency tracking and analytics inside simulation systems:
-
Systems now track performance metrics in real time (e.g. time to action, error rates, decision patterns), enabling personalized remediation.
-
Health simulation research updates in 2025 highlight metrics like biometrics, team training analytics, and performance dashboards being increasingly studied.
-
In medical education, simulation-based training has been repeatedly shown to improve clinical performance, boost learner confidence, and reduce errors in real patient care.
By integrating analytics, institutions can assess whether learners meet proficiency thresholds before advancing—improving safety and educational quality.
4. Portability, Low-Resource Adaptation & Accessibility
One limitation of traditional simulation labs is cost, space, and logistical constraints. The 2025 trend is toward portable, modular, in-situ simulation, even in low-resource settings:
-
Portable simulation solutions (mobile labs, tablet-based debrief tools, compact manikins) let training happen in clinical wards, remote hospitals, or field settings.
-
Simulation research now also emphasizes facilitating simulation in low-resource or rural settings.
-
With global demand rising (see market projections below), there will be pressure for scalable, lightweight simulators that deliver core functionality without massive infrastructure.
5. Market Growth, Strategic Investment & Institutional Adoption
These technological trends are backed by robust market and institutional momentum:
-
According to a global medical simulation strategic report, the market was valued at US$8.7 billion in 2024 and is forecast to reach US$19.5 billion by 2030 (CAGR ~14.5 %)
-
Another source estimates the healthcare simulation market (2024) at USD 1.65 billion, projecting growth to USD 4.17 billion by 2030 with ~16.8 % CAGR.
-
Markets & Markets projects in 2025 already about USD 3.5 billion and growing to USD 7.23 billion by 2030 (CAGR ~15.6 %)
-
Institutions are increasing investments in upgraded simulation centers. For instance, Methodist Healthcare is investing in a $2.7M upgrade to expand simulation labs with advanced mannequins, remote viewing, and debrief spaces.
These numbers reflect that simulation is no longer niche — it is becoming core to medical education worldwide.
6. Focus on Interprofessional & Team Training
Beyond training individuals, there’s growing emphasis on team-based simulation:
-
In real clinical environments, care is rarely individual; simulation is increasingly used to train interprofessional teams (nurses, physicians, allied health) in crisis resource management, communication, coordination.
-
The HealthySimulation research updates highlight team training as a key ongoing focus in simulation studies (2025)
-
This approach helps learners not only master technical skills but also non-technical skills (communication, leadership, situational awareness).
Why These Trends Matter — The Advantages
Together, these trends promise to address longstanding challenges of medical training:
-
Efficiency & scalability: AI scenario generation and analytics reduce faculty load and allow more practice per learner.
-
Safety: Learners can make errors in simulation, not with patients.
-
Flexibility & accessibility: Portable and digital simulators allow training where & when needed.
-
Data-driven improvement: With analytics, curricula can be refined based on real performance data.
-
Interoperability: Blended systems (virtual + physical) allow staged learning and cost control.
-
Global reach: Low-resource adaptations make simulation feasible in emerging markets.
Simulation-based medical education (SBME) is now widely recognized as a core pedagogical tool, not just an adjunct.
How You Can Leverage These Trends (for Suppliers / Educators / Buyers)
If your organization is considering simulation solutions, here are strategic moves worth considering:
-
Offer modular systems — support virtual + physical components, allow incremental upgrades.
-
Embed AI / LLM tools — scenario authoring, branching logic, instant feedback capabilities.
-
Provide analytics dashboards — track learner metrics, compare cohorts, support accreditation.
-
Design portability — lightweight, mobile, suitable for in-situ / point-of-care settings.
-
Support team-based modes — multi-user simulation, networked scenarios.
-
Focus on cost-effectiveness — aim for lower TCO (total cost of ownership) and remote support.
-
Offer trial / pilot programs — let institutions test with limited risk.
-
Align with research & standards — simulation research continues to refine best practices (e.g. SQUIRE-SIM guidelines)
References
-
Arxiv (2024) Automated Generation of High-Quality Medical Simulation Scenarios. Available at: https://arxiv.org/abs/2404.19713.
-
Arxiv (2025a) MedSimAI: AI-driven patient simulation platform for medical training. Available at: https://arxiv.org/abs/2503.05793.
-
Arxiv (2025b) Patient-specific dynamic digital-physical twin for coronary intervention training. Available at: https://arxiv.org/abs/2505.10902.
-
HealthySimulation (2025a) 7 Future Trends in Healthcare Simulation Training. Available at: https://www.healthysimulation.com/7-future-trends-healthcare-simulation-training.
-
HealthySimulation (2025b) Healthcare Simulation Research Update – May 2025. Available at: https://www.healthysimulation.com/healthcare-simulation-research-update-may-2025.
-
Globenewswire (2025) Healthcare Medical Simulation Strategic Research Report 2025 – Global Market to Reach $19.5 Billion by 2030. Available at: https://www.globenewswire.com/news-release/2025/02/25/3032203/28124/en/Healthcare-Medical-Simulation-Strategic-Research-Report-2025-Global-Market-to-Reach-19-5-Billion-by-2030-Growing-Focus-on-Patient-Safety-and-Clinical-Training-Drives-Demand.html.
-
Grand View Research (2024) Healthcare / Medical Simulation Market Size, Share & Trends Analysis Report 2024-2030. Available at: https://www.grandviewresearch.com/industry-analysis/medical-healthcare-simulation-market.
-
Markets and Markets (2025) Healthcare / Medical Simulation Market by Product & Service – Global Forecast to 2030. Available at: https://www.marketsandmarkets.com/Market-Reports/healthcare-medical-simulation-market-1156.html.
-
Express News (2025) Methodist Healthcare to invest $2.7M in advanced nurse simulation lab upgrades. Available at: https://www.expressnews.com/business/article/san-antonio-methodist-healthcare-nurses-training-21067694.php.
-
ScienceDirect (2024) Advances in digitally-based medical simulation and online education. Available at: https://www.sciencedirect.com/science/article/pii/S2405844024116581.
-
Taylor & Francis Online (2025) Simulation-based medical education (SBME): current evidence and future directions. Available at: https://www.tandfonline.com/doi/full/10.1080/10872981.2025.2469779.
-
PubMed Central (2024) Simulation-based training improves clinical performance and learner confidence: a systematic review. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC11224887.