In the fast-paced world of healthcare, an essential nursing equipment list serves as a foundation for best care practices. Nurses rely on specific tools to monitor patients, administer medications, and ensure safety. Each item plays a crucial role in daily operations. Without proper equipment, the quality of care may falter, leading to potential harm.
Consider the stethoscope, a symbol of nursing professionalism. It allows nurses to assess heartbeats and lung sounds, offering immediate insights. Yet, not every nurse has the latest model or the skills to use it effectively. This disparity highlights the importance of ongoing training and access to updated equipment.
Moreover, essential tools like IV pumps and personal protective gear can vary greatly between settings. Some healthcare facilities struggle to maintain adequate supplies, risking patient safety. An effective nursing equipment list must address these gaps and adapt to evolving healthcare needs. By prioritizing access to essential tools, we enhance our ability to provide high-quality, reliable care.
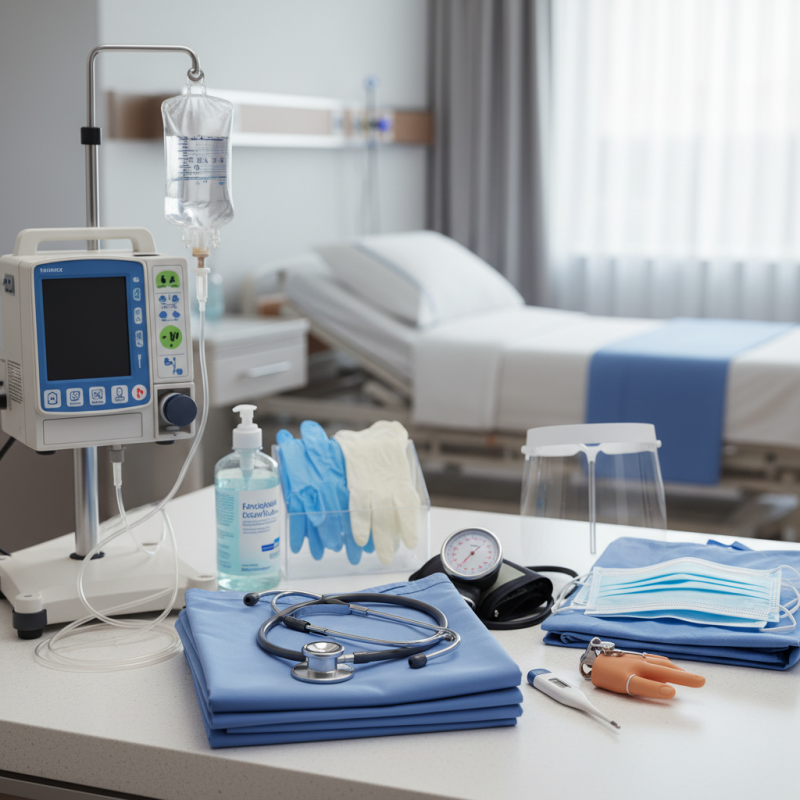
Nurses play a crucial role in patient care. Their toolkit is essential for ensuring safety and effective treatment. Basic supplies include gloves, masks, and hand sanitizers. These items help prevent infections and maintain hygiene. A stethoscope is vital for assessing heart and lung sounds. It’s a timeless tool in every nurse's arsenal.
However, possessing tools is just the beginning. Understanding their use is equally important. For instance, a thermometer is not just for measuring temperature. It assists in monitoring a patient’s progress and detecting fevers. Sometimes, nurses encounter challenges with equipment. For example, a malfunctioning blood pressure cuff can lead to incorrect readings. Reflecting on these moments enhances problem-solving skills.
Moreover, technology is reshaping nursing tools. Electronic health records streamline patient information but can be overwhelming. Training is vital to navigate these systems effectively. Adapting to change and refining skills is a continuous journey for nurses. This will enhance patient care and personal growth in their profession.
| Equipment | Purpose | Usage |
|---|---|---|
| Stethoscope | To listen to heart and lung sounds | Used for routine examinations and monitoring |
| Thermometer | To measure body temperature | Essential for assessing fever or infection |
| Sphygmomanometer | To measure blood pressure | Used for routine check-ups and critical assessments |
| Glucometer | To check blood glucose levels | Important for diabetes management |
| Oxygen Saturation Monitor | To monitor oxygen levels in the blood | Critical for respiratory assessments |
| IV Catheter | For intravenous therapy | Administer medications and fluids |
Patient assessment and monitoring are critical components in nursing practice. Key equipment plays a vital role in ensuring accurate evaluations. Devices like sphygmomanometers for blood pressure measurement and stethoscopes for heart and lung sounds are foundational. According to the World Health Organization, effective monitoring can reduce patient complications by up to 25%.
Basic vital signs monitors are essential for tracking crucial indicators. These include heart rate, temperature, and respiratory rate. Data from the American Nurses Association highlights that timely monitoring can significantly improve patient outcomes. However, it’s important to acknowledge the limitations of these tools. Overreliance on technology may lead to missed assessments that only a nurse’s intuition can catch.
Pulse oximeters are increasingly used to assess oxygen saturation levels, yet they aren't infallible. False readings can occur due to poor circulation or motion artifacts. Additionally, clinical training often emphasizes the use of these devices. However, many nurses occasionally lack confidence in interpreting the data. Continuous education and practice are vital for developing the required skills.
This chart illustrates the importance of various nursing equipment used in patient assessment and monitoring, highlighting the frequency of usage in clinical settings.
Infection control is paramount in nursing. Without the right supplies, healthcare quality diminishes. According to the Centers for Disease Control and Prevention (CDC), infection can increase patient morbidity and mortality rates. Proper supplies reduce these risks effectively.
Essential supplies include personal protective equipment (PPE), gloves, masks, and hand sanitizers. These items create a barrier against pathogens. Studies indicate that using PPE reduces the transmission of infectious diseases by up to 70%. However, not all facilities consistently implement these protocols, leading to gaps in infection control.
Regular training on the use of these supplies is crucial. Staff must understand when and how to use PPE to maintain safety. Yet, many nurses report feeling unprepared. A report by the World Health Organization (WHO) revealed that nearly 40% of healthcare workers lack proper training in infection control measures. This gap points to a need for enhanced education and resource allocation in healthcare settings.

Patient comfort and safety are paramount in nursing care. Essential equipment plays a crucial role in fostering a healing environment. According to the Agency for Healthcare Research and Quality, well-chosen patient care equipment can reduce incidents of accidents and improve recovery times.
Key items include supportive positioning devices, such as pillows and wedge cushions. These tools help maintain proper patient alignment. They reduce the risk of pressure ulcers significantly. A study by the National Pressure Injury Advisory Panel indicated that effective use of positioning aids can cut pressure injury rates by up to 40%.
Furthermore, safety features like bed rails and non-slip mats enhance care. They prevent falls, which are a leading cause of injury in healthcare settings. The Centers for Disease Control and Prevention reports that falls result in over 700,000 hospitalizations each year. Nonetheless, some healthcare providers may underestimate the importance of regular equipment assessments. Inadequate attention to maintaining these essentials can lead to lapses in patient care. This oversight highlights the need for continuous education and training in using care equipment effectively.
In nursing practice, effective documentation and communication tools are vital for delivering quality care. A study by the Agency for Healthcare Research and Quality (AHRQ) highlights that nearly 80% of sentinel events result from poor communication. Clear and accurate documentation can significantly reduce these incidents.
Nurses use various tools to enhance communication. Electronic health records (EHRs) are now standard in many hospitals. They allow for real-time updates and shared access among healthcare providers. A 2022 report by the National Institute of Health found that EHR implementations improve patient safety by reducing medication errors by up to 30%. However, reliance on technology can sometimes hinder personal interactions. Nurses may feel they have less time for patient engagement due to data entry demands.
Another crucial aspect is handoff communication. Inconsistent practices during shift changes can lead to significant gaps in patient care. The Joint Commission emphasizes structured communication tools, such as SBAR (Situation, Background, Assessment, Recommendation), to enhance clarity during handoffs. Even with these methodologies, lapses still occur, indicating a need for continuous training and improvement. Balancing technology and personal touch remains a challenge in nursing.