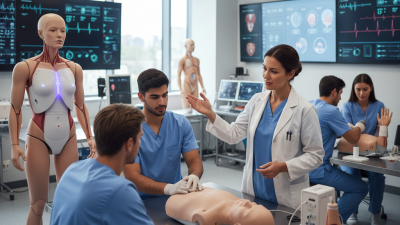
In the realm of medical training, the creation of effective Patient Simulation Scenarios is crucial. These scenarios provide a unique environment where future healthcare professionals can practice their skills. By simulating real-life situations, trainees can enhance their decision-making and technical abilities.
Crafting realistic Patient Simulation Scenarios requires careful consideration. Trainers must identify common challenges in healthcare. The scenarios should reflect actual patient situations and allow for varied responses. Creating a scenario may seem simple, but it often reveals gaps in knowledge or unexpected complexities. Trainers should encourage reflection on these imperfections.
Effective Patient Simulation Scenarios also need to engage trainees emotionally. Realistic scenarios can evoke stress or anxiety, mirroring true medical settings. This emotional component can enhance learning, making it memorable. However, trainers must balance realism with support to prevent overwhelming students. Developing effective scenarios is an ongoing process that requires adjustment and improvement based on feedback.
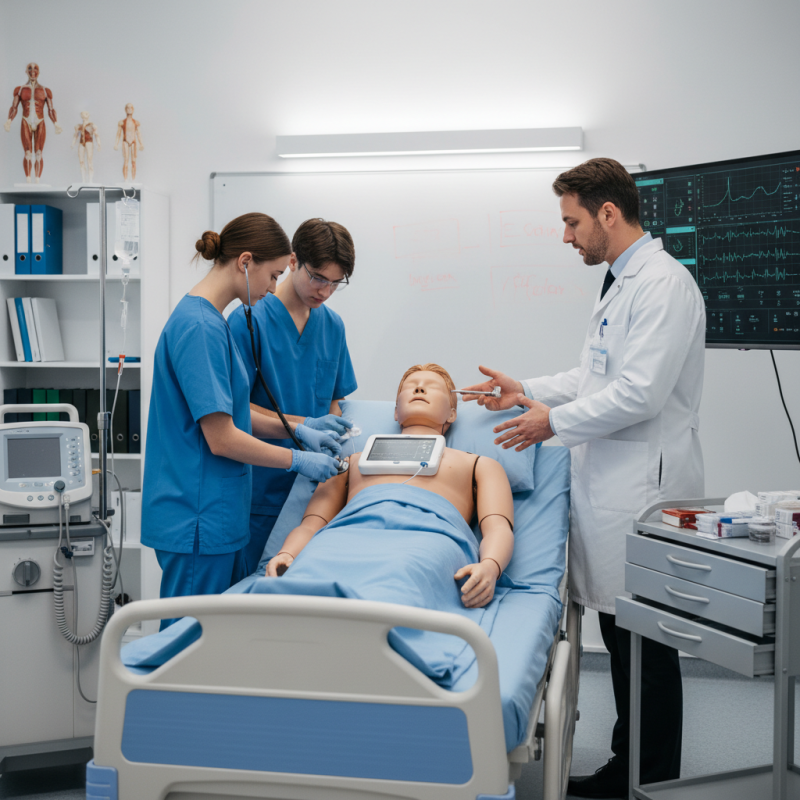
Identifying training objectives is crucial for creating effective patient simulation scenarios in medical training. A well-defined objective sets the foundation for the training experience. It ensures that learners know what skills and knowledge they should acquire from simulations. According to a recent report, 75% of medical educators believe that clear objectives enhance learning outcomes.
When formulating objectives, consider both clinical skills and soft skills. An objective could focus on improving diagnostic accuracy or enhancing communication with patients. It’s also vital to involve interdisciplinary teams in the objective-setting process. This can lead to broader insights. Engaging various healthcare roles encourages a well-rounded approach to patient care.
However, not all scenarios meet expectations. Some studies indicate that only 60% of training scenarios align with real-world challenges. This gap can stem from overly generic objectives or lack of clinical relevance. Training may not reflect actual patient interactions. Continuous evaluation and feedback from participants can refine objectives. Using participant experiences for future scenarios is necessary for improvement.
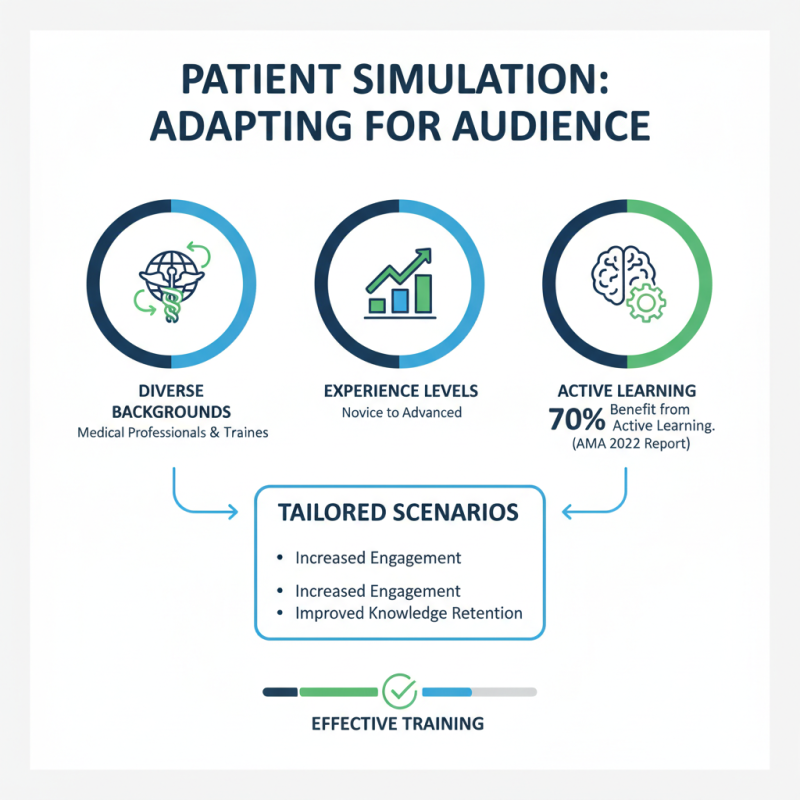
Understanding the target audience is crucial for creating effective patient simulation scenarios. Medical professionals come from diverse backgrounds and possess varying levels of experience. According to a 2022 report by the American Medical Association, around 70% of medical trainees benefit from active learning environments. Tailoring scenarios to meet these unique needs enhances engagement and retention.
It's important to pinpoint the specific skills each group must develop. For instance, novice practitioners might focus on basic bedside manners and history-taking. In contrast, seasoned professionals may need advanced decision-making simulations. Evidence suggests that 60% of advanced learners preferred scenarios that challenge their existing knowledge. Incorporating unexpected complications can foster critical thinking, yet some scenarios still fall short of delivering realistic challenges.
Creating realism is easier said than done. Actors may not always replicate patient behavior accurately, which can mislead learners. Additionally, the lack of diverse patient cases can limit exposure to varying conditions. Addressing these gaps is essential for effective training. A study revealed that 40% of medical trainees felt unprepared for certain clinical situations, highlighting the need for thoughtful scenario design. Listening to feedback is as important as the initial concept.
Designing effective patient simulation scenarios requires a deep understanding of clinical guidelines. These guidelines provide a framework for creating realistic and relevant training experiences. Start by identifying key clinical scenarios that healthcare professionals frequently encounter. Scenarios such as emergency responses or chronic disease management can be particularly impactful. Utilize detailed patient histories and realistic symptoms to enhance authenticity. Include diverse patient backgrounds to reflect real-world complexity.
Consider incorporating errors or complications within scenarios. This approach pushes learners to think critically and make decisions under pressure. For example, a scenario could present an unexpected allergic reaction. Participants must assess the situation and respond swiftly. It can be uncomfortable, but it fosters vital skills. Discussing these imperfect scenarios afterward encourages reflection and learning.
Pay attention to the environment in which simulations occur. A well-designed space that mimics an actual clinical setting can significantly improve the training experience. Props, such as medical equipment and charts, add to the realism. However, remember that it’s essential to balance realism with educational purpose. Avoid overwhelming participants with unnecessary details that divert focus. Effective simulation is an iterative process, requiring continuous refinement and feedback from participants to enhance future scenarios.
Integrating technology into patient simulation scenarios is crucial for effective medical training. With advancements in virtual reality, augmented reality, and artificial intelligence, training becomes more immersive. According to a report from the National Center for Biotechnology Information, simulation-based learning improves retention rates by up to 70%. This statistic highlights the importance of integrating modern tools to enhance learning outcomes.
Interactive simulation environments allow for real-time feedback and scenario adjustments. For instance, using high-fidelity mannequins can replicate real-life emergencies. Trainees can practice critical skills in a safe space. However, not all simulations yield optimal results. A study showed that poorly designed scenarios may confuse learners rather than educate them. Feedback must be precise to address misconceptions effectively.
Additionally, accessibility must be a focus. Some institutions struggle to provide advanced tools due to budget constraints. A 2020 survey indicated that 55% of training programs faced financial limitations. It’s essential to balance technology integration with available resources. This ensures a comprehensive approach to medical training, fostering enhanced learning experiences.
Evaluating the outcomes of simulation training sessions is crucial for effective medical training. It allows educators to assess both skills and knowledge retention in participants. After each session, sharing constructive feedback is essential. This practice not only helps trainers refine their methods but also allows learners to identify their strengths and areas for improvement.
Collecting data from participants is a valuable step. Surveys or focused discussions can provide insights into the learning experience. However, not all feedback will be positive. Some learners may feel unprepared for real-life scenarios. It’s important to address these concerns and adapt training accordingly. Engaging in reflective practice, where trainers review their scenarios and learning outcomes, can reveal gaps in the training process. This ongoing evaluation helps ensure that simulation training is truly effective.
Ultimately, the goal is to create meaningful and realistic scenarios. Yet, achieving this balance can be challenging. There may be a tendency to over-simplify complex medical situations. It’s critical to challenge this approach. Regularly revisiting and updating simulation scenarios ensures they reflect current medical practices. Engaging students in this process fosters a collaborative learning environment.